Jackson Health Foundation Announces $100 Million Raised to Support New Emergency Room at Jackson Memorial Hospital
Jackson Health Foundation Announces $100 Million Raised to Support New Emergency Room at Jackson Memorial Hospital

What:
Jackson Health Foundation announced a record-breaking $100 million to support Jackson Memorial Hospital’s new emergency room, opening to the public on April 23. The fundraising amount marked a major historic milestone in Jackson Health System’s philanthropic history.
The fundraising milestone comes at a critical time, as demand for emergency services across Miami-Dade County continues to rise. This historic milestone was made possible through the generosity of several community leaders, philanthropists, partner organizations, and the community at large. Additionally, during One Day for Jackson (April 16, 2026), Jackson Health Foundation’s annual day of giving, nearly $900,000 (and counting) was raised to support crucial initiatives across Jackson Health System, including the new emergency room at Jackson Memorial Hospital. The Jackson Health Foundation will continue fundraising until April 30.
The special event honored the donors and community leaders who helped make the new emergency room at Jackson Memorial – one of the largest in the nation – a reality. The expansion to South Florida’s largest public healthcare system will further strengthen Jackson’s ability to provide timely, efficient, and high-quality care to all who need it, regardless of their ability to pay.
Built by Skanska, the new, 178,000-square-foot emergency room is three times the size of the current one and is designed to deliver faster, more efficient, and patient-centered care.
“I know you’re not supposed to pick favorites, but the idea of a new emergency room serving as a beacon of hope and healing on this bustling campus in Miami-Dade County’s health district truly energized me. From the very beginning, this project had a special sense of purpose and the potential to be the most transformative at Jackson in a generation,” said Carlos Migoya, CEO of Jackson Health System. “Jackson Health Foundation has never received any single gift larger than $10 million, so $100 million didn’t just feel ambitious, it felt impossible. To our founding benefactors, thank you for coming together, not for the credit of any one individual, but in the spirit of a true collective effort that benefits the health and well-being of our entire community. What we celebrate today is not just what has been built, but everything that will be possible within these walls, and beyond.”
The event featured remarks from Carlos Migoya, CEO of Jackson Health System; Flavia Llizo, CEO of Jackson Health Foundation; Miami-Dade County Mayor Daniella Levine Cava; City of Miami Mayor Eileen Higgins, and key donors who contributed to the construction of the facility.
Guests also enjoyed exclusive and immersive guided tours of the newly completed facility and Jackson-inspired libations.
The founding partners that have pledged donations to this new facility include the Lennar Foundation, the Miller Foundation, Benjamin Leon Jr. Charitable Foundation, Related Group, Royal Caribbean Group Foundation, the Kadre Family, José Milton Foundation, the Batchelor Foundation, Trish and Dan Bell, Codina Family, the Gorson family, Harold Marzouka Jr., and Françoise Marzouka Family Trust. Additional philanthropists have also pledged their support, including the Guiribitey family, Mr. David Pyle, and Chaim Katzman, to name a few.
“This new emergency room represents what’s possible when generosity, vision, and a shared commitment to accessible, high-quality care come together. We’re incredibly grateful to our supporters and founding partners for helping us build the next era of emergency care in Miami-Dade County, right here at Jackson,” said Flavia Llizo, CEO of Jackson Health Foundation. “This is a milestone not only for Jackson, but for our community – it’s a powerful reminder of what we can accomplish together in Miami. This new emergency room at Jackson Memorial Hospital reflects our shared commitment to delivering exceptional care when it matters most.”
Key features of the new emergency room include:
- Private patient rooms for comfort and privacy
- Fast-track triage areas to reduce wait times
- 57 observation rooms and four advanced resuscitation rooms for critical cases
- Family lounges and private waiting areas to support loved ones
The new emergency room, located at 1026 NW 19th St., spans two city blocks and includes designated parking and a patient drop-off area.
From Stroke to Strength: A Jackson Memorial Hospital Employee’s Road to Recovery
From Stroke to Strength: A Jackson Memorial Hospital Employee’s Road to Recovery








By Carla Palmer
For more than 25 years, Sean Riley has supported Jackson Memorial Hospital in a variety of roles — from mental health to landscaping — today, he works in supply chain, helping ensure the hospital has what it needs to care for patients. His routine was simple: a 15-minute scooter ride to work, followed by a short walk to his office — located, as it would turn out, just beneath Ryder Trauma Center at Jackson Memorial.
On June 30, 2025, that routine was suddenly interrupted.
After three days of feeling dizzy and not himself, Riley woke up on a Monday morning planning to go to work as usual. Over the weekend, he had fallen off his scooter while riding with friends at a slow speed, brushing it off as dehydration. But when his symptoms didn’t improve, he made a small but crucial decision: instead of riding his scooter, he drove the less than 10 minutes to the hospital “just in case.”
As soon as he walked inside, Riley noticed something was very wrong. He kept drifting to one side, and the room felt like it was spinning. His supervisor immediately recognized the signs and had him admitted for testing.
The diagnosis: ischemic stroke.
An ischemic stroke happens when a blood vessel in the brain becomes blocked, cutting off the blood supply. It accounts for about 87 percent of cases, making it the most common stroke type.
“I had damaged nerve endings on the right side of my brain, which caused loss of function on the left side of my body,” Riley said.
Soon after arriving at Jackson Memorial, he began losing feeling on the left side of his body — just the beginning of a long recovery journey.
“I almost completely lost all function on my left side. I couldn’t move my leg, my foot, my arm,” Riley said. “You know it’s there, but you can’t do anything with it.”
Doctors treated and monitored him closely for several days, managing his blood pressure and ensuring he wasn’t bleeding heavily before he could begin rehabilitation. On the third day, he was transferred to Christine E. Lynn Rehabilitation Center for The Miami Project to Cure Paralysis at UHealth/Jackson Memorial, where his recovery officially began.
There, Riley worked with occupational and physical therapists Monday through Friday, determined to regain his movement.
“Sean came in with a lot of energy, which is very difficult to have at this stage,” said Ariana Gutierrez, Riley’s occupational therapist. “I went in every morning at 7:30 a.m. — most of my patients don’t want to wake up that early — but he was already ready to go. We were the first people in the gym every day.”
When Riley first arrived, he couldn’t lift his arm over his head. Movements that once felt automatic had become impossible on the left side of his body. While his speech and facial movement were unaffected, Riley was determined to regain full function. He worked day and night with that goal in mind.
That dedication made all the difference.
“By the time he left inpatient rehab, I knew he was ready for outpatient therapy — and I knew he was going to excel,” Gutierrez said.
After discharge, Riley began outpatient therapy, working closely with Jill Munro and other physical therapists.
The focus shifted to rebuilding strength and endurance.
“When he came in, he wasn’t able to run or do many of the things he could do before,” Munro said. “We worked on strengthening, and eventually, he was able to jog on the treadmill at a pretty decent speed for long periods of time.”
His therapy included squats, step-ups, calf raises, leg presses, and other strength-building exercises.
“For every session I had with her, I would leave sweating,” Riley said. “She really helped bring me back.”
Both Munro and Gutierrez agree that what set Riley apart was his attitude.
“He’s a go-getter,” Munro said. “He did everything we asked him to do, he is a super motivated human.”
“Having the attitude Sean had makes all the difference,” Gutierrez added.
Today, Riley is back at work, once again walking the Jackson Memorial corridors — a testament to early recognition, comprehensive care, and his relentless determination.
“Everybody did what they were supposed to do to get me to where I’m at today,” Riley said. “I can be nothing but thankful.”
Hope Before Birth: Key West Family Celebrates First In-Utero Spina Bifida Repair at Holtz Children’s Hospital
Hope Before Birth: Key West Family Celebrates First In-Utero Spina Bifida Repair at Holtz Children’s Hospital






By: Krysten Brenlla
Emily Shipman, 35, shares an inseparable bond with her 8-year-old daughter, Bella. Alongside her husband, the two do everything together – from managing their family’s small mom-and-pop shop in their hometown of Key West to traveling the world.
That bond grew even stronger when Bella got the news she had always hoped for: a baby sibling was on the way.
“My daughter and I left for Italy on May 28, 2024, and we were going to be gone the whole month of June,” Shipman said. “It was June 1 when I found out I was pregnant.”
Shipman and her family were excited for their newest addition. But, an 18-week ultrasound appointment in Key West showed a concerning diagnosis that changed everything.
“I just remember that the ultrasound tech kept looking at something, and she went to go get the doctor,” Shipman said. “The doctor came in, looked at the ultrasound, and told me that my baby had spina bifida. I didn’t even know what that meant.”
Spina bifida is a condition that happens when a baby’s spine doesn’t form properly during early pregnancy, leaving part of the spinal cord exposed to the outside. Normally, the spine closes around the spinal cord like a protective tube. But in spina bifida, the spine stays open and exposes the spinal cord, which can cause problems with the spinal cord, nerves, and the brain, leading to issues with movement, sensation, and even brain development.
“Within one minute, I was told that I wasn’t going to have a normal child, and that my baby would more than likely be wheelchair-bound,” Shipman said. “It was pretty much painted that I was going to have a vegetable baby.”
Despite the devastating diagnosis, Shipman never gave up hope. Her OB-GYN referred her to a maternal-fetal medicine specialist, who explained that an in-utero spina bifida repair might be possible.
That’s when Shipman met Rodrigo Ruano, MD, PhD, director of UHealth Jackson Fetal Care Center and division chief of UHealth Jackson Maternal-Fetal Medicine, and Heather McCrea, MD, PhD, director of pediatric neurosurgery at Holtz Children’s Hospital, and a UHealth – University of Miami Health System pediatric neurosurgeon.
Together, they lead the only maternal-fetal medicine/pediatric neurosurgery team to provide fetal spina bifida repair in South Florida. Dr. Ruano cares for the mother and exposes the baby in utero, and Dr. McCrea repairs baby’s spinal defect while they remain in the uterus.
“In Emily’s case, we also performed an MRI and found that the baby had hindbrain herniation, which is a condition where part of the brain is pushed down into the opening at the base of the skull,” Dr. McCrea said. “That pressure can block spinal fluid and affect brain function. After reviewing her case, Dr. Ruano and I determined that she was a strong candidate for fetal surgery.”
“We typically offer in-utero repair of spina bifida between 22 and 26 weeks of pregnancy,” Dr. Ruano added. “The mother is placed under general anesthesia, and through a small C-section-like incision, we open the uterus and carefully expose the baby’s back. A pediatric neurosurgeon, in this case Dr. McCrea, then closes the defect. This procedure can significantly improve the baby’s brain structure and reduce the risk of further nerve damage or fluid buildup in the brain.”
Shipman and her family decided to move forward with the procedure. On October 22, 2024, she became the first patient to undergo in-utero spina bifida repair at Holtz Children’s.
Just two months later, on December 31, 2024, Shipman and her family rang in the New Year with their newborn son, Luey. When he was born, his back was completely closed, and the hindbrain abnormality was fixed.
Luey received specialized care in the Newborn Intensive Care Unit (NICU) at Holtz Children’s Hospital, where a dedicated team of neonatologists, nurses, and specialists ensured he had the strongest start possible.
“It’s very unique that God gave me this opportunity to help those babies before they’re born,” Dr. Ruano said.
As Luey grows, he’s receiving care by Dr. McCrea and a multidisciplinary team in the Holtz Children’s Comprehensive Spina Bifida Clinic.
“We’re really excited to see who Luey becomes, and what he does,” Shipman said. “We’re also so excited to see the impact the fetal surgery had on him. I can’t thank the teams at Jackson Memorial and Holtz Children’s enough.”
A Brother’s Gift Helps Young Boy Beat Cancer Twice with Help from Holtz Children’s Hospital
A Brother’s Gift Helps Young Boy Beat Cancer Twice with Help from Holtz Children’s Hospital








By: Krysten Brenlla
At just 14, Jake Alexander Kleppen is known on Instagram as a “victorious warrior” – a title he’s earned by facing cancer not once, but twice.
“I never felt any symptoms – all we noticed was my eye,” he said. “It was swelling a lot, and I was originally diagnosed with hypertropia when I was 8.”
Hypertropia is a condition where one eye turns upward. But when Jake’s pediatrician took a closer look, she noticed something was off. She sent him to the emergency room for testing, where doctors made a life-changing discovery.
“He was actually suffering from Ewing sarcoma,” said Marisel Jarrin Kleppen, Jake’s mother. “Never did I imagine we would leave the hospital with a cancer diagnosis.”
Ewing sarcoma is an aggressive soft tissue cancer that usually appears in the limbs, hips, or chest. For Jake, it appeared in his eye, which is extremely rare.
“At that point, he was already stage three,” Marisel said. “Had we waited any longer, who knows what would’ve happened.”
Thankfully, in September 2019, Jake found a specialized pediatric cancer team at Holtz Children’s Hospital.
“We targeted his cancer with 11 months of chemotherapy and 31 rounds of proton beam radiation, which is very precise,” Marisel said. “It affected the symmetry of his face, vision, teeth, and even cognition. But still, he fights through that – he’s super smart and never gives up.”
Eventually, Jake rang the bell at Holtz Children’s – he was cancer-free. He returned home to his family and friends, celebrating nearly five years of remission.
“I felt so free – I felt amazing,” Jake said.
But toward the end of 2024, after a week at Civil Air Patrol camp, Jake felt sick.
“I gave him Advil, and told him to go to sleep. The next morning, he woke up in a puddle of sweat,” Marisel said. “I knew immediately that we had to go to the hospital.”
In December, Jake was diagnosed with his second form of cancer – leukemia, a blood and bone marrow cancer where abnormal white blood cells crowd out the healthy ones, making it hard for the body to fight infections, stop bleeding, or carry oxygen.
“They did the blood test, and they noticed that his white blood cells were basically non-existent,” Marisel said. “All his numbers were low, and in my head, I didn’t want to think it was cancer. But I just knew it wasn’t normal.”
Jake was referred back to Holtz Children’s to fight cancer a second time.
“Unfortunately, the leukemia was caused by the treatments he received to fight off his original cancer,” said David Crawford, MD, director of pediatric stem cell transplantation at Holtz Children’s and UHealth – University of Miami Health System. “But Jake will be a unique child who survives two different malignancies.”
His new treatment plan included chemotherapy and a targeted drug called blinatumomab, which uses the body’s immune system to attack leukemia cells, in hopes of reaching remission.
Once Jake was in remission, the search for a bone marrow donor began – and against all odds, his brother, Justin, was a perfect match.
“The first time Jake was diagnosed with cancer, I was devastated,” Justin said. “I couldn’t believe he had to go through this a second time, but I knew I had to stay strong. When I found out I was a match to be his bone marrow donor, I was so excited.”
On May 12, 2025, after months of preparation that included immunotherapy, chemotherapy, and full-body radiation, Jake was ready for his bone marrow transplant.
“Being Jake’s donor is going to give us a bigger and better bond, and I’m just excited for him to get better afterward,” Justin said.
“Having Justin as my donor means we’re really blood bonded now,” Jake said. “I’m so grateful.”
Within six weeks, Jake’s team hopes he’ll be able to go home. And within a year, they’re optimistic he’ll fully recover with a new immune system from his brother.
“At Holtz Children’s, we have outstanding pediatric cancer care and cutting-edge treatment options,” Dr. Crawford said. “Jake and his family are wonderful people – we’re hopeful that he’ll survive this and feel like himself again.”
“I tell other kids who may be going through something similar to always see the good in everything,” Jake said. “It’s not going to be easy, but always try to find the silver lining, and you’ll be okay. I know I will.”
Fifteen Years and Counting: How a Kidney Transplant from the Miami Transplant Institute Saved Young Boy’s Life
Fifteen Years and Counting: How a Kidney Transplant from the Miami Transplant Institute Saved Young Boy’s Life



By: Krysten Brenlla
When Chase Cooper, 20, was just 2 years old, he was diagnosed with a congenital kidney and urinary tract condition. One of his kidneys was filled with cysts – a condition called multicystic dysplastic kidney.
Additionally, the other kidney had a blockage where the ureter, a thin tube that carries urine from each kidney to the bladder, didn’t develop normally.
“My family knew from the minute I was born that I would have problems with my kidneys,” Cooper said. “They knew that I’d eventually need a transplant.”
To find the best treatment options, his family sought care at the Miami Transplant Institute (MTI), an affiliation between Jackson Health System and UHealth – University of Miami Health System.
After an extensive evaluation, the multidisciplinary team found that Cooper was eligible for a kidney transplant, and he was placed on the list.
For 10 months, he received at-home peritoneal dialysis. However, on a Wednesday evening in 2010, Cooper’s family got the call they longed for – there was a match.
Five-year-old Cooper and his loved ones rushed to Jackson Memorial Hospital, where he underwent his kidney transplant, performed by Gaetano Ciancio, MD, chief medical officer and director of the kidney and kidney-pancreas transplant programs at MTI.
The surgery marked the beginning of a new chapter, but it was far from the end of Cooper’s medical journey.
“Even if someone has a healthy kidney after transplant, the medical process doesn’t stop,” he said. “Taking care of it is one thing, but sustaining it for 15 to 20 years is the real challenge.”
However, despite the obstacles throughout his life, the team at MTI has been Cooper’s guiding force.
“Chase’s case is remarkable – many pediatric transplant recipients require multiple transplants over the years, yet Chase’s kidney has lasted an impressive 15 years,” said Marissa Defreitas, MD, a pediatric nephrologist at MTI. “However, the challenges extend beyond the kidney itself. As a side effect of the anti-rejection medications, Chase developed diabetes, along with gastrointestinal complications.
Despite these hurdles, he continues to push forward with the unwavering support of his family and the team at Jackson and MTI.”
As he grew older, Cooper began to advocate about the urgent need for organ donors, speaking at school events and debate tournaments. Throughout his kidney transplant journey, he also developed a passion for encouraging young people to register as organ donors.
“I think every day about the people on the transplant list who need an organ – just like I needed a kidney,” Cooper said. “It’s a tremendous gift – I wouldn’t know where I’d be if I didn’t get that kidney. That’s what Jackson does best – they give people another opportunity to live life to the fullest.”
Now a political science major at Lynn University, Cooper’s committed to making a difference. He hopes to continue advocating for organ donation through community efforts and speaking engagements.
“During Donate Life Month in April, I tell people – check the box. You can save eight lives in one day,” Cooper said. “We need more people who are willing to donate because too many people are waiting for their second chance.”
Woman Regains Mobility After Parkinson’s Diagnosis Through Specialized Therapy at Jackson North
Woman Regains Mobility After Parkinson’s Diagnosis Through Specialized Therapy at Jackson North

By: Krysten Brenlla
Sandra Senkow has always embraced an active lifestyle – she loves the outdoors, riding bikes, and spending time with her family.
Two years ago, Senkow’s life took an unexpected turn when she began experiencing symptoms that would later lead to a Parkinson’s disease diagnosis.
“It all started after knee surgery when my boyfriend noticed subtle changes in my movements,” Senkow said.
With a family history of Parkinson’s, the 59-year-old was concerned. She sought medical advice, undergoing a series of tests before receiving a definitive diagnosis.
The news was a shock, but Senkow was determined to face the challenge head-on.
“My symptoms primarily affected my walking,” she said. “My aunt had Parkinson’s disease, so when I got the diagnosis, I knew I needed to be proactive to manage the condition.”
With the help of her family, Senkow explored various treatment options, including Lee Silverman Voice Treatment (LSVT), a specialized, high-intensity program designed to help people with Parkinson’s improve their movement and speech by retraining the brain with specific repetitive exercises.
After some research, her family found the LSVT program at Jackson North Medical Center, where she met her physical therapist, Sabrina Cherelus.
“When I first saw Sandra, she exhibited common Parkinson’s symptoms, including rigidity, slowed movement, and walking impairments, like uneven steps,” Cherelus said. “Although she hadn’t experienced falls, she was still a fall risk. That’s when we decided LSVT BIG would be a great intervention for her.”
LSVT BIG is a program designed to help patients with Parkinson’s and other neurological conditions regain movement control. Over the course of four weeks— four sessions per week— Senkow worked with physical therapists on different exercises, which incorporated seven daily exercises that were tailored to her needs.
“The LSVT BIG exercises are designed to retrain the brain and create new pathways to compensate for Parkinson’s-related impairments,” Cherelus said. “Sandra was incredibly consistent and motivated. She kept up with her home exercises and always came in ready to show her progress.”
By the end of her therapy, Senkow had achieved measurable results. She transitioned from a medium fall risk to a low fall risk, regained her natural walking ability, and returned to walking four to five miles regularly.
“It was night and day from when she started,” Cherelus said. “She not only met her goals, but also gained a tool to manage her symptoms. Parkinson’s is a lifelong condition, but with science, technology, and therapy, we can help patients maintain their mobility and independence for longer.”
“I want to keep Parkinson’s at bay as long as I can by staying active and using the techniques they taught me,” Senkow added. “The therapy was fantastic, and Sabrina was great. I’d tell anyone with Parkinson’s to sign up for LSVT—it makes a real difference.”
Man Diagnosed with Rare Autoimmune Disease Beats the Odds with Life-Saving Lung Transplant at Miami Transplant Institute
Man Diagnosed with Rare Autoimmune Disease Beats the Odds with Life-Saving Lung Transplant at Miami Transplant Institute









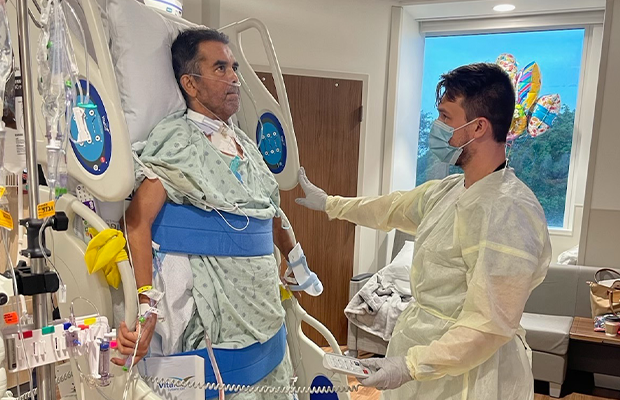
By: Miranda Torres
“You probably will never have children”, are words Richardy Blanchard, 40, heard in her early 20’s after being diagnosed with polycystic ovarian syndrome. After two decades of irregular menstrual cycles, she was shocked to discover she was pregnant.
Due to her diagnosis and age, Blanchard began seeing a high-risk maternal fetal medicine doctor along with her OB-GYN to create a prenatal care plan. During a routine check-up at 18 weeks, the ultrasound tech discovered Blanchard had an incompetent cervix, meaning her cervix was too short to support a pregnancy.
The doctor told Blanchard, “This is an inevitable abortion and you’ll be lucky if he survives another week. But we’ll catch it next time for your next pregnancy.”
“He didn’t know everything it took for me to get to this point to be a mom,” Blanchard said. “It was so dismissive.”
Blanchard sought a second opinion and found The Women’s Hospital at Jackson Memorial. After reading a patient testimonial about a mother who gave birth to two healthy babies after having a cervical cerclage, or procedure to help keep the cervix closed, she knew The Women’s Hospital team would be equipped to care for her and her baby.
At 19 weeks, Blanchard began having unusual discharge and visited the emergency room at Jackson Memorial Hospital. The doctor explained that because of her open cervix, her amniotic sack was protruding, posing a risk for sepsis, a potentially lethal reaction to an infection that can lead to organ failure. The options included inducing labor, which would mean the baby would be stillborn, or leaving the hospital because her pregnancy was not yet viable. It was then she met Devita Price, APRN, director of professional practice at The Women’s Hospital.
“As a healthcare professional, I empowered her to listen to her gut and her body and reminded her we are here to help along the way and keep her educated on ALL her options,” Price said.
Blanchard decided to go home and trust that God would make a way for her to have this baby.
During her ER visit, Blanchard also met Pouya Abhari, MD, FACOG, a maternal fetal medicine specialist at The Women’s Hospital. Dr. Abhari promised that once Blanchard reached 22 weeks gestation, the earliest stage of viability for a baby, he would admit her and care for her until it was time to deliver her baby.
Once she was admitted at 22 weeks, Blanchard’s cervix was already 3 centimeters dilated.
The high-risk team was monitoring her and her baby daily for signs of preterm labor and infection.
Additionally, a counsellor was brought in several times to speak with Blanchard and address her mental wellbeing. Maternal mental health is a priority at Jackson, especially among Dr. Abhari’s team at The Women’s Hospital.
“We want mothers to feel like they are still being focused on and taken care of as a person, outside of being an expectant mom,” Dr. Abhari said.
At 30 weeks, Blanchard’s water broke and she went into labor naturally. The Holtz Children’s Hospital NICU team was present during the labor to ensure her baby would receive the necessary care from the moment he entered the world.
“The synergy between the delivery and NICU team was something I had never seen before. It was perfect, I couldn’t have dreamed of a more perfect birth,” Blanchard said.
Samuel Gerdes was born healthy, answering all of Blanchard’s prayers.
“When I held my son, I felt God was with me,” she said. “I was holding him while he was crying, and I felt so grateful for the gift of being a mom.”
While in the NICU, Samuel never required oxygen and took to bottle feeding quickly with donor milk, allowing him to gain weight and reach his milestones. Blanchard spent every available moment by his side.
“Being a first-time parent and this being her miracle baby, she was a great advocate and had thoughtful questions,” said Rebecca Jones, MD, a NICU hospitalist at Holtz Children’s. “For us it’s something we do every day but for these parents, it’s something they experience just one in their lifetime, so it’s important for us to give them time and space to take it all in and answer all their questions.”
Two months later, Samuel was discharged, finally going home to be surrounded by his family.
“Throughout this journey, I have experienced the best and worst of the healthcare industry,” Blanchard said. “Thank you to every doctor who answered my questions, celebrated every day with me, learned my son’s name, and embodied God’s love.”
Defying the Diagnosis: A Journey to First-time Motherhood at The Women’s Hospital at Jackson Memorial
Defying the Diagnosis: A Journey to First-time Motherhood at The Women’s Hospital at Jackson Memorial
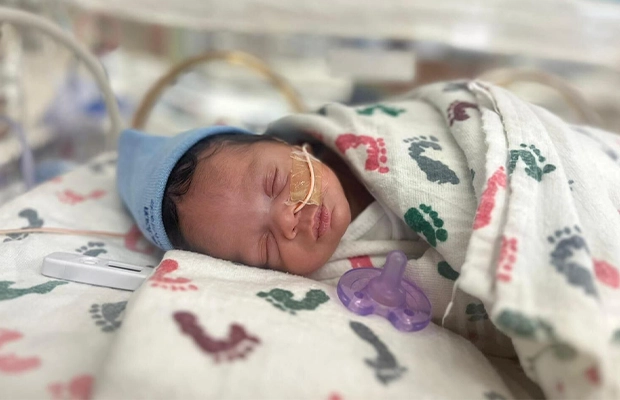



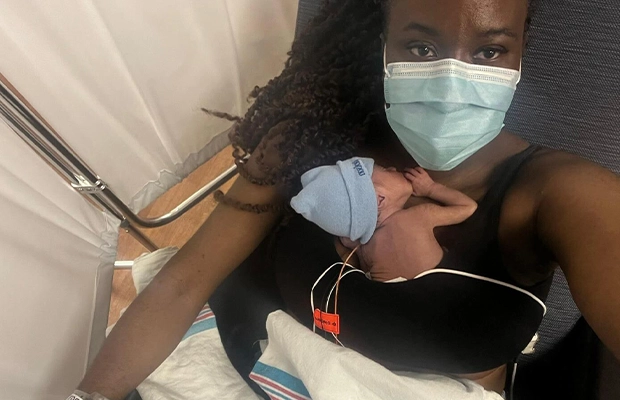

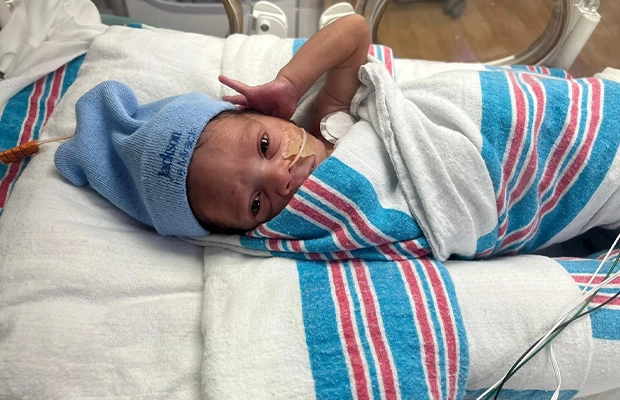
By: Miranda Torres
“You probably will never have children”, are words Richardy Blanchard, 40, heard in her early 20’s after being diagnosed with polycystic ovarian syndrome. After two decades of irregular menstrual cycles, she was shocked to discover she was pregnant.
Due to her diagnosis and age, Blanchard began seeing a high-risk maternal fetal medicine doctor along with her OB-GYN to create a prenatal care plan. During a routine check-up at 18 weeks, the ultrasound tech discovered Blanchard had an incompetent cervix, meaning her cervix was too short to support a pregnancy.
The doctor told Blanchard, “This is an inevitable abortion and you’ll be lucky if he survives another week. But we’ll catch it next time for your next pregnancy.”
“He didn’t know everything it took for me to get to this point to be a mom,” Blanchard said. “It was so dismissive.”
Blanchard sought a second opinion and found The Women’s Hospital at Jackson Memorial. After reading a patient testimonial about a mother who gave birth to two healthy babies after having a cervical cerclage, or procedure to help keep the cervix closed, she knew The Women’s Hospital team would be equipped to care for her and her baby.
At 19 weeks, Blanchard began having unusual discharge and visited the emergency room at Jackson Memorial Hospital. The doctor explained that because of her open cervix, her amniotic sack was protruding, posing a risk for sepsis, a potentially lethal reaction to an infection that can lead to organ failure. The options included inducing labor, which would mean the baby would be stillborn, or leaving the hospital because her pregnancy was not yet viable. It was then she met Devita Price, APRN, director of professional practice at The Women’s Hospital.
“As a healthcare professional, I empowered her to listen to her gut and her body and reminded her we are here to help along the way and keep her educated on ALL her options,” Price said.
Blanchard decided to go home and trust that God would make a way for her to have this baby.
During her ER visit, Blanchard also met Pouya Abhari, MD, FACOG, a maternal fetal medicine specialist at The Women’s Hospital. Dr. Abhari promised that once Blanchard reached 22 weeks gestation, the earliest stage of viability for a baby, he would admit her and care for her until it was time to deliver her baby.
Once she was admitted at 22 weeks, Blanchard’s cervix was already 3 centimeters dilated.
The high-risk team was monitoring her and her baby daily for signs of preterm labor and infection.
Additionally, a counsellor was brought in several times to speak with Blanchard and address her mental wellbeing. Maternal mental health is a priority at Jackson, especially among Dr. Abhari’s team at The Women’s Hospital.
“We want mothers to feel like they are still being focused on and taken care of as a person, outside of being an expectant mom,” Dr. Abhari said.
At 30 weeks, Blanchard’s water broke and she went into labor naturally. The Holtz Children’s Hospital NICU team was present during the labor to ensure her baby would receive the necessary care from the moment he entered the world.
“The synergy between the delivery and NICU team was something I had never seen before. It was perfect, I couldn’t have dreamed of a more perfect birth,” Blanchard said.
Samuel Gerdes was born healthy, answering all of Blanchard’s prayers.
“When I held my son, I felt God was with me,” she said. “I was holding him while he was crying, and I felt so grateful for the gift of being a mom.”
While in the NICU, Samuel never required oxygen and took to bottle feeding quickly with donor milk, allowing him to gain weight and reach his milestones. Blanchard spent every available moment by his side.
“Being a first-time parent and this being her miracle baby, she was a great advocate and had thoughtful questions,” said Rebecca Jones, MD, a NICU hospitalist at Holtz Children’s. “For us it’s something we do every day but for these parents, it’s something they experience just one in their lifetime, so it’s important for us to give them time and space to take it all in and answer all their questions.”
Two months later, Samuel was discharged, finally going home to be surrounded by his family.
“Throughout this journey, I have experienced the best and worst of the healthcare industry,” Blanchard said. “Thank you to every doctor who answered my questions, celebrated every day with me, learned my son’s name, and embodied God’s love.”
Pediatric Transplant Team Give Central Florida Teenager a Second Chance at Life at Holtz Children’s Hospital
Pediatric Transplant Team Give Central Florida Teenager a Second Chance at Life at Holtz Children’s Hospital







By: Miranda Torres
When Brianna Denny was 11 years old, she was diagnosed with a blood factor deficiency, a rare bleeding disorder where clotting proteins in the blood are missing, low, or don’t work well. Until this point, she was a normal, healthy kid who enjoyed softball, spending time with her friends and family, and going to school.
In February, Brianna, now 15, broke out in a rash on her feet. When it began to spread to her legs and became painful to the touch, she and her family knew something was wrong. A visit to a local children’s hospital led her to a rheumatologist, who began running tests to identify the cause of the rash.
About a month later, the rash returned and went further up Brianna’s leg. A hematologist recommended she be transported to Holtz Children’s Hospital.
While at Holtz Children’s, it was discovered that Brianna had autoimmune hepatitis, a rare, chronic liver disease that occurs when the body’s immune system attacks the liver, and hepatopulmonary syndrome, a rare lung complication connected to liver disease. Due to these conditions, she was experiencing stage three cirrhosis of the liver, a condition that can only be treated with a liver transplant.
Her hepatopulmonary disease meant that Brianna required oxygen for over a month while the team at Holtz children’s focused on her liver.
Brianna was immediately placed under the care of the pediatric transplant team at the Miami Transplant Institute (MTI), which included Jennifer Garcia, MD, medical director of pediatric transplant services, adult and pediatric intestinal rehabilitation, and intestinal transplant, Akin Tekin, MD, liver, intestinal, and multivisceral surgeon, and Jessica Hochberg, MD, pediatric gastroenterologist at Holtz Children’s Hospital.
Brianna was listed for a transplant on April 17, and just seven days later, received the call that a liver had been found. On April 25, the team transplanted Brianna and gave her a second chance at life.
While it was initially expected that Brianna could potentially require oxygen for at least a year post-transplant, she is off oxygen and recovering back home in Lake Placid. “She is determined, a fighter, and against all odds wants to get back to her normal life which is think is hugely important in her recovery journey,” says Dr. Hochberg. She also has a great support system in her family.”
She is looking forward to returning to her favorite activities such as softball and spending time with her friends, and school in November.
“Thank you to the team of doctors, nurses, and everyone at the hospital who took care of me,” Brianna said. “My mom gave me the strength to get through this, and so did my friends, who reached out every day.”
Columbus Student and Cross County Star Suffers Massive Brain Bleed, Makes Full Recovery at Jackson
Columbus Student and Cross County Star Suffers Massive Brain Bleed, Makes Full Recovery at Jackson








By: Krysten Brenlla
When Matthew Nunez was a freshman at Christopher Columbus Senior High School, he followed his older brother’s footsteps by joining the track and cross-country teams.
For years, the now 18-year-old competed in countless races without any issues. As his senior year approached, Matthew was preparing to run at the collegiate level, backed by his family, friends, and teammates.
“It was really a normal day, a typical race day on a Friday afternoon,” said Matthew’s parents, Anna and Carlos Nunez. “In fact, he was pumped up for the race and ready for it. He had absolutely zero signs of anything.”
On Friday, September 27, 2024, less than half a mile into the race, Matthew started to feel sharp pain on the right side of his head that spread down to his jaw.
“The pain got so bad that I had to turn myself around and walk toward the golf cart that follows the runners,” Matthew said.
At first, the race paramedics thought it was dehydration or heat exhaustion. However, as they started to examine him, they knew something else was wrong.
“I usually wait for him at the two-mile mark, but I noticed that Matthew wasn’t coming,” Anna said. “People began calling me, telling me, ‘Something happened, you have to get back to the rescue at the finish line.’”
Matthew was rushed to Ryder Trauma Center at Jackson South, where a team led by Antonio Marttos, MD, a UHealth – University of Miami Health System trauma surgeon at Ryder Trauma, worked to stabilize and assess him.
“When he arrived at Jackson South, he was in critical condition,” Dr. Marttos said. “What concerned us most was that he was not moving his right side properly. We quickly sent him in for a CT scan to evaluate for a possible brain bleed, but within minutes, at the CT scanner, his heart and lungs began to fail.”
The multidisciplinary care team acted quickly and intubated Matthew, placing him on a ventilator to help him breathe and giving him life-saving medication to help his heart keep adequate blood pressure and blood flow to the brain.
When the CT scan was finally performed, a massive brain bleed was found.
“I was in the chapel at Jackson South when Dr. Marttos gave me the news. It was just utter shock,” Anna said. “So many thoughts started popping into my head. But, Dr. Marttos and his team gave us the confidence we needed, and I knew that they would do everything they could to help our son.”
To control the bleed, Matthew underwent emergency neurosurgery, which lowered the pressure on his brain that was triggering multi-organ failure. Once resuscitated, he was airlifted to Ryder Trauma Center at Jackson Memorial.
At Jackson Memorial, a specialized team of neurosurgeons was ready to take over and address the source of Matthew’s bleeding.
“The initial step was ensuring his heart and lungs were resuscitated,” said Adib Abla, MD, chief of cranial neurosurgery at Jackson Memorial. “Ultimately, we found the cause of bleeding in the brain was a vascular lesion located in the brainstem, which is an abnormality in the brain’s blood vessels that can burst, resulting in a dangerous brain bleed.”
On October 4, Dr. Abla and his team performed a successful surgery that removed the entire lesion.
After surgery, Matthew spent 26 days in the intensive care unit, and 11 days at Christine E. Lynn Rehabilitation Center for The Miami Project to Cure Paralysis at UHealth/Jackson Memorial.
“Everybody here made those days as smooth and comfortable as could be considering the situation – they made us feel at home,” Carlos said. “I knew that Matthew was going to be okay because he was in the best place possible to recover from this. It is an absolute miracle.”
Today, Matthew has made a full recovery, and has returned to what he loves the most – running. He’s looking forward to finishing his senior year, and hopes to continue his running career in college.
“To the entire team at Jackson, there are no words that can truly express my gratitude,’” he said. “They saved my life.”